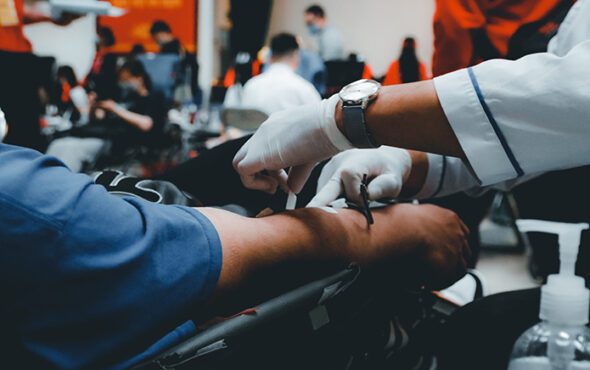
When his mother fell ill, Karan, a 25-year-old gay man from New Delhi, hurried to donate blood. But as he filled out the mandatory form for donors, he realised he would be turned away because of his sexuality and made a snap decision.
Karan, the only member of his family with the same blood group as his mother, decided to lie about being gay, potentially risking prosecution.
“I was … scared of being caught (but) at that time, the only thing that mattered to me was my mother,” said Karan, whose full name is not being published to protect his identity.
“It was only later that I realised it was so dehumanising, harmful to my dignity and a breach of my privacy as a queer person in this country,” Karan told Openly.
India’s current laws prohibit trans people, gay and bisexual men, and female sex workers from donating blood, despite acute shortages in the world’s most populous country and a global shift away from bans on blood donation by LGBTQIA+ people.
The rules, which date back to the start of the HIV/AIDS crisis in the 1980s, exclude members of those groups on the grounds that they are at high risk for the virus – even though all donated blood is screened for HIV.
An estimated 2.5 million people are living with HIV in India according to UNAIDS. Among Trans Indian, 3.8% are living with the virus, while 3.3% of men who have sex with men have HIV.
It is mandatory for donors to be free from diseases that are transmissible by blood transfusion, and the donor should not be at any risk “for HIV, Hepatitis B or C infections”.
But critics, who say the policies excluding LGBTQIA+ people were determined by fear and discrimination rather than medical science, are calling on the government to follow other countries and scrap the ban.
“The government argues on the basis of sexual behaviour of the community but that puts all transgender people under the same blanket and that’s not okay,” said Santa Khurai, a transgender activist from the northeastern state of Manipur.
Khurai filed a petition to the Supreme Court in 2021 that challenged the constitutional validity of two clauses of the blood donation policy, but the government has defended its guidelines, stating that they were based on scientific fact.
Khurai is awaiting the date of the next hearing in the case.
India’s Health Ministry, the National AIDS Control Organisation (NACO) and the National Blood Transfusion Council (NBTC) – government bodies which oversee blood donation – did not respond to requests for comment.
Global shift
LGBTQIA+ rights campaigners say India is falling behind on the issue as countries around the world scrap restrictions on LGBTQIA+ blood donors.
This year, the U.S. Food and Drug Administration, which administers the country’s blood supply, lifted curbs on gay and bisexual men donating blood, following similar measures in Canada, France, Greece, Britain and Germany.
They say the devastating impact of the COVID-19 pandemic in India spotlighted the need for reform.
“Several queer people struggled to get donors from their community due to the ban,” said Aqsa Shaikh, associate professor of community medicine at Hamdard Institute of Medical Science and Research.
Shaikh, who is trans, said it was “not only unscientific but also illogical” to ban all trans people from donating blood even when they might not participate in higher risk activities such as sex work or penetrative sex.
Because of India’s blood shortages, many patients have to rely on family members to donate.
For LGBTQIA+ people, many of whom are estranged from their families due to their sexuality or gender identity, the current restrictions make it impossible for them to receive donations from their partners or friends within the community instead.
Delhi-based lawyer and bioethicist, Rohin Bhatt was unable to donate blood and plasma for his friend’s husband who was in hospital with COVID in 2021, despite undergoing regular testing for sexually transmitted infections.
“The government’s policy can’t be to marginalise and impose a blanket ban but to improve their testing policies for blood donors. I am not a disease vector,” said Bhatt, who identifies as a non-binary queer person.
It is already mandatory in India to test every unit of donated blood for HIV/AIDS as well as Hepatitis B, Hepatitis C, syphilis and malaria.
Anant Bhan, a public health researcher at Sangath, a mental health nonprofit, said the current policy of excluding LGBTQIA+ donors was misguided.
“Inclusivity should be a key element of government health programmes, and can focus on individualised risk-assessment rather than a blanket one based on gender identity,” he said.
If India’s Supreme Court decides to allow same-sex marriage in a case currently being heard at the top court, the blood donation rules would look even more outdated, campaigners say.
“If same-sex marriage is legalised, what happens when a married gay man needs blood to save his life? His partner won’t be able to donate blood because of these guidelines,” said Khurai.
Critics say the issue demonstrates persistent discrimination faced by LGBTQIA+ people in India five years since the country decriminalised homosexuality by scrapping part of Section 377, a law introduced by India’s former British colonial rulers that had stood for almost 160 years.
“This ban is discriminatory,” Bhan said. “(It) also precludes their ability to donate blood which is an essential life-saving resource.”
Reporting by Jaishree Kumar and Aman Singh.
GAY TIMES and Openly/Thomson Reuters Foundation are working together to deliver leading LGBTQIA+ news to a global audience.



